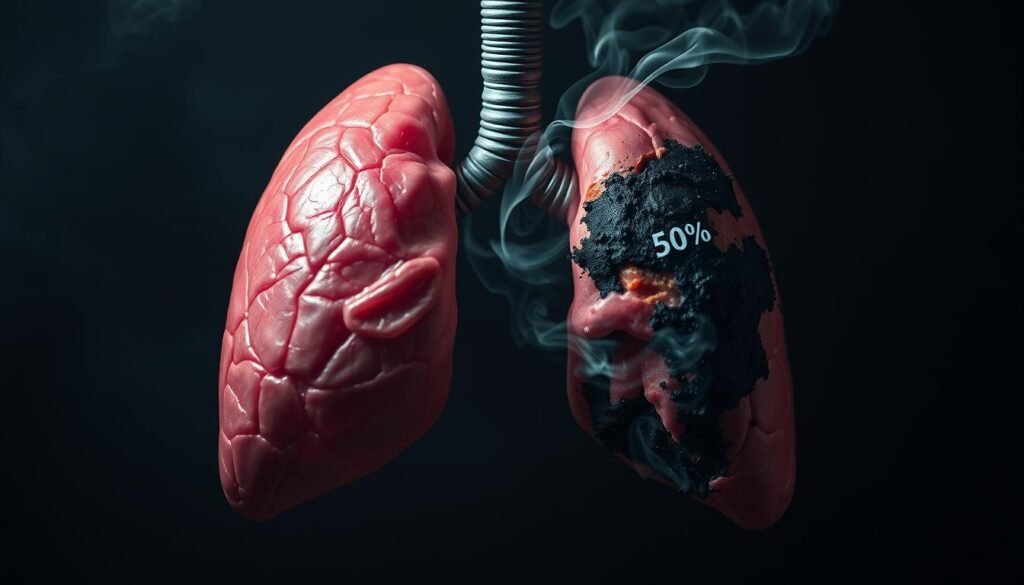
Cigarette smoking causes 80% to 90% of all lung cancer cases. This fact shows the big effect smoking has on health. Smokers have up to a 30 times higher risk of getting lung cancer compared to nonsmokers. This shows just how big a role smoking plays in lung cancer.
Yet, 15% to 25% of lung cancer happens in people who never smoked. This means that other factors also contribute to lung cancer, not just smoking. In this article, we look at what affects lung cancer risk. We also share stats that show the clear differences between smokers and nonsmokers.
Key Takeaways
- 80% to 90% of lung cancer cases are attributed to smoking.
- Smokers are up to 30 times more likely to develop lung cancer than nonsmokers.
- Approximately 15% to 25% of lung cancer cases occur in lifelong never-smokers.
- Cessation of smoking can lead to a significant increase in life expectancy.
- Secondhand smoke poses risks for nonsmokers, contributing to lung cancer cases.
Understanding Lung Cancer
Lung cancer is a serious problem. It starts as a tumor in the lungs. Often, people don’t show symptoms early on. This makes early diagnosis tough and knowing the risks important.
Smoking heavily links to lung cancer. It causes 80% to 90% of lung cancer deaths in the U.S. Smokers are 15 to 30 times more likely to get lung cancer. This shows why cancer tests and keeping healthy lungs are vital.
Other risks include radon gas, asbestos, and air pollution. These can cause not just lung cancer but other types too. It’s essential to check these factors closely.
Lung cancer comes in two main types. They are non-small cell lung cancer and small cell lung cancer. Each type acts differently and needs its own treatment plan.
To learn more about lung cancer and how to prevent it, check out understanding lung cancer.
Statistics on Lung Cancer Prevalence
Lung cancer is a top health issue worldwide, leading in cancer deaths. Every year, about 1.8 million people die from it. In the U.S., it causes more deaths than breast, prostate, and colorectal cancers combined. By 2024, it’s expected we’ll see about 234,580 new cases and about 125,070 people will die from it.
Looking closer, 10% to 15% of lung cancers are small cell lung cancer (SCLC). The rest, 80% to 85%, are non-small cell lung cancer (NSCLC). Most people diagnosed are over 65, with the average age at 70. Everyone has a chance of getting lung cancer, but it’s roughly 1 in 16 for men and 1 in 17 for women.
- 1 in 5 cancer deaths are caused by lung cancer in the U.S.
- Black men are 12% more likely to get lung cancer than White men.
- Black women have a 16% lower chance of getting it than White women.
- New lung cancer cases are dropping, thanks to more people stopping smoking.
The decline in lung cancer rates in men has been seen for decades; for women, it’s been notable in the last ten years. However, survival rates really depend on the cancer type and when it’s found.
| Statistic | Value |
|---|---|
| Estimated Annual Lung Cancer Deaths (U.S.) | 125,070 |
| Projected New Cases in 2024 (U.S.) | 234,580 |
| Percentage of Small Cell Lung Cancer | 10% to 15% |
| Percentage of Non-Small Cell Lung Cancer | 80% to 85% |
| Lifetime Risk for Men | 1 in 16 |
| Lifetime Risk for Women | 1 in 17 |
The Impact of Smoking on Lung Cancer Risk
Tobacco use is a major health crisis because it’s closely linked to lung cancer. Smoking is responsible for nearly 90% of lung cancer cases in men and 70% to 80% in women. Smokers are 30 times more likely to get lung cancer than non-smokers.
Lung cancer accounts for 31% of cancer deaths in men and 26% in women in the U.S. This fact shows how serious the situation is.
Each year, lung cancer causes over 160,000 deaths in the United States. It takes more lives than several major cancers combined. The survival rate five years after diagnosis is only 15%. This underlines how deadly lung cancer is.
Carcinogens in tobacco smoke cause mutations that can lead to lung cancer. This process, called field cancerization, changes the lungs of smokers. Even former smokers face an increased risk of lung cancer because of these changes.
Smoking changes how genes work and affects cells beyond the lungs. It plays a role in lung cancer’s resistance to treatment. This makes the effects of smoking even more dangerous.
Smoking is the top risk factor for lung cancer. Secondhand smoke also poses a big risk, being the third leading cause of lung cancer in the U.S. Knowing this highlights how vital it is to stop smoking.
How Much Higher is the Risk of Lung Cancer in Smokers than in Nonsmokers?
It’s vital to know how smoking affects lung cancer risk. Smoking greatly increases lung cancer risk. This is backed by numerous smoking statistics.
Lung Cancer Rates Among Smokers
Smokers have a high chance of getting lung cancer. For men, it’s about 14.8% and for women, 11.2%. Nonsmokers have a risk of just 1.8%. This shows how smoking significantly raises lung cancer risk.
Around 80% to 90% of lung cancer deaths are due to smoking. Smokers are 15 to 30 times more likely to get or die from lung cancer than nonsmokers. Even those who smoke a little are at risk, hinting at the importance of quitting.
Statistics for Nonsmokers
But, nonsmokers can also get lung cancer, with 10% to 20% being diagnosed. Secondhand smoke, radon, air pollution, and workplace chemicals are major risk factors. Studies suggest that nonsmokers with lung cancer have more mutations related to cancer. This points to serious health issues even without smoking.
For more on risks from secondhand smoke, visit lung cancer in former smokers.
| Group | Lung Cancer Risk | Contributing Factors |
|---|---|---|
| Smokers (Males) | 14.8% | Smoking, secondhand smoke, radon, air pollution |
| Smokers (Females) | 11.2% | Smoking, environmental toxins, workplace exposure |
| Nonsmokers | 1.8% | Radon, secondhand smoke, air pollution, genetic mutations |
Secondhand Smoke: An Underestimated Risk Factor
Secondhand smoke is a big problem for public health. It often gets overlooked when we talk about lung cancer risks. This smoke comes from burning tobacco products and puts dangerous chemicals into the air. People who don’t smoke can still face serious health problems from it. This includes a higher chance of getting lung cancer.
Health Risks Associated with Secondhand Smoke
It’s impossible to ignore the effects of secondhand smoke. For people exposed to it, the chance of getting lung cancer is 1.35 times higher than for those who aren’t. Never smokers who come into contact with this smoke are nearly 1.69 times more likely to develop lung cancer. This shows how risky it is to be around smokers, especially if there’s a lot of smoke.
- Being around secondhand smoke for 2–3 hours a day makes lung cancer 2.27 times more likely.
- If you’re exposed for more than three hours every day, the risk goes up to 2.29 times.
- Non-smokers who live with smokers face a 26% higher risk of lung cancer.
- A review of 37 studies found passive smoking increases lung cancer risk by 26%.
This information underlines the importance of being aware of secondhand smoke’s dangers. Even short exposures can harm non-smokers. It’s essential to find ways to reduce this health risk everywhere.
Other Risk Factors for Lung Cancer
Lung cancer isn’t just a smoker’s issue. It also hits those who’ve never touched a cigarette. Factors like environmental factors and genes matter a lot. Knowing these risks helps us fight cancer better.
Environmental Exposures
Where you live and work can affect your lung cancer risk. Radon gas is a big danger, especially for non-smokers. It’s the second top cause of lung cancer in the U.S. Research shows radon is a major threat if you don’t smoke.
Being around asbestos is risky too, mainly for miners and mill workers. Living near busy roads ups the risk because of air pollution. Scientists have found a clear link to more lung cancer cases.

Genetic Predisposition
Your family’s health history affects your lung cancer risk. If lung cancer runs in the family, you’re more likely to get it. This is due to certain genes. These genes can make cells in your lungs grow oddly.
A diet full of fruits and veggies might lower the danger. Even if your genes make you more likely to get lung cancer.
Types of Lung Cancer in Smokers vs Non-Smokers
Lung cancer includes many types. A person’s smoking history greatly influences these. The type of tumor in smokers versus nonsmokers shows important differences in how they are diagnosed and treated.
Common Subtypes in Smokers
Smokers often get certain lung cancers, especially:
- Squamous Cell Carcinoma
- Small Cell Lung Cancer
These lung cancers come from tobacco smoke’s harmful effects. Squamous cell carcinoma starts in the lungs’ central area. On the other hand, small cell lung cancer spreads fast and is very aggressive.
Adenocarcinoma in Nonsmokers
Adenocarcinoma is the most common lung cancer in nonsmokers. It makes up about 93% of lung cancer in these people. This type forms in the lungs’ outer parts and can come from things like radon gas and secondhand smoke.
Adenocarcinoma makes treating cancer more complex due to its unique traits. Smokers face different lung cancers than nonsmokers, who have their own challenges and treatment options.
| Type of Lung Cancer | Common in Smokers (%) | Common in Nonsmokers (%) |
|---|---|---|
| Squamous Cell Carcinoma | High | Rare |
| Small Cell Lung Cancer | High | Rare |
| Adenocarcinoma | Low | 93 |
Knowing the differences in lung cancer types shows why personalized treatment and early detection are crucial for smokers and nonsmokers.
Age and Gender Disparities in Lung Cancer Diagnosis
It’s critical to know how age and gender affect lung cancer diagnosis. This helps in making prevention and treatment better. Smokers usually find out they have lung cancer at 66 years old. Nonsmokers get diagnosed at about 67 years old. These differences show how biology and environment affect lung cancer risk.
Age at Diagnosis for Smokers
Studies point to a worrying trend in lung cancer diagnoses among smokers. They often receive their diagnosis around the same age. This information helps public health initiatives aimed at lowering lung cancer rates. Research underlines the importance of early diagnosis in smokers, especially when looking at ages.
Gender Differences in Lung Cancer Incidence
There’s a big difference in lung cancer rates between men and women, thanks to changing smoking habits. Surprisingly, over half of women with lung cancer don’t smoke, unlike most men. This demands a deeper look into risks, especially among the young. Young women are now more likely to get lung cancer than young men. This calls for better awareness and specific actions.
| Gender | Percentage of Lung Cancer Diagnosed | Percentage of Never-Smokers | Average Age at Diagnosis |
|---|---|---|---|
| Women | 50% | Up to 50% | 67 years |
| Men | Majority | 15-20% | 66 years |
These findings about age and gender shine a light on what healthcare providers need to do. They have to focus on age and gender in diagnosing lung cancer. By doing so, they can help those at greater risk.
The Role of Carcinogens in Tobacco Products
Tobacco products are full of harmful chemicals like formaldehyde, benzene, and certain nitrosamines. These chemicals raise the chance of getting lung cancer. Because cigarettes have these carcinogens, smokers are always in contact with dangerous substances. This leads to serious health problems over time.
Nicotine Addiction and its Impact
Nicotine addiction keeps people using tobacco, which means they’re always near carcinogens. When someone gets hooked on nicotine, they’re more likely to use tobacco. Knowing how carcinogens cause cancer can help us find ways to stop people from smoking. For example, they can damage DNA and cause mutations. This damage often leads to lung cancer, showing why stopping tobacco use is critical. For more information, check this link on carcinogens in tobacco products.
| Carcinogen | Health Effects |
|---|---|
| Formaldehyde | Respiratory issues, increased cancer risk |
| Benzene | Bone marrow damage, increases leukemia risk |
| Nitrosamines | DNA damage, lung cancer |
| Polonium-210 | Radiation exposure, lung cancer |
| Aromatic amines | Bladder cancer, lung cancer |
Treatment Approaches for Lung Cancer Patients
Lung cancer treatment is different for smokers and nonsmokers. This is because their diseases and health conditions vary. Understanding these treatments helps in getting the best results for patients.
Targeted Therapies for Non-Smokers
Targeted therapies work well for nonsmokers, especially when we find certain genetic changes. Finding mutations like EGFR helps in planning the treatment. These newer therapies have improved the control of lung cancer. They also lead to longer survival for nonsmokers.
Standard Treatments for Smokers
Smokers usually get more common treatments such as surgery, chemotherapy, and radiation. The treatment considers the cancer’s stage, patient’s health, and the type of lung cancer. Since smoking is a top cause of lung cancer, these patients often have more advanced disease. They need a detailed treatment plan made just for them.
| Treatment Type | Smokers | Nonsmokers |
|---|---|---|
| Surgery | Common for localized cancers | Less frequent, often combined with targeted therapies |
| Chemotherapy | Standard approach for advanced cases | Utilized based on histological findings |
| Radiation | Adjuvant therapy after surgery | Rare, more common in advanced or recurrent cases |
| Targeted Therapies | Limited response without specific mutations | Highly effective with certain mutations present |
Different treatment approaches for smokers and nonsmokers highlight the need for personalized care. Tailoring treatment to a patient’s smoking history leads to better outcomes. And it improves life quality for patients with lung cancer.
Conclusion
The gap in lung cancer risk between those who smoke and those who don’t is huge. Smoking plays a huge part in the rise of cancer rates. In Tianjin, from 2010 to 2019, there were 82,769 new cases of lung cancer. Many of these were in people who smoked or used to smoke.
This fact shows how crucial it is to push for ways to prevent lung cancer. This includes helping people quit smoking. Also, we must teach about the dangers of direct smoking and being around smoke.
Teaching people is key to bringing down the number of lung cancer cases. It is important to start campaigns. These should teach the risks of smoking and being near smoke. Also, we should push for regular check-ups to catch cancer early. This is especially true for non-smokers, where we often find adencarcinoma, a type of lung cancer.
Interestingly, 64.15% of non-smokers who got lung cancer were women. This shows a change that we need to focus on.
To wrap up, we all need to work together to tell people about keeping healthy. We need good policies to prevent lung cancer and support for those trying to stop smoking. By tackling these risks directly, we can fight lung cancer. This will make society healthier and help everyone affected by this tough disease.