Did you know about 60% of people with lung cancer get radiation therapy sometime during treatment? This large number shows how important radiation therapy is for treating conditions like non-small cell lung cancer (NSCLC). Radiation therapy is key in killing cancer cells. But, it’s important for patients to know about the risks. They should understand that the treatment can have several side effects.
For those whose tumors are too big or in tricky places for surgery, radiation therapy might be the only choice. It’s often used after surgery to get rid of leftover cancer cells. It can also be used before surgery to make tumors smaller. Patients might run into different types of radiation therapy, like external beam radiation therapy (EBRT) and brachytherapy. Knowing about the possible side effects is crucial. Being informed helps patients get ready for their treatment. It also helps them talk more with their doctors.
Key Takeaways
- About 60% of lung cancer patients receive radiation therapy.
- Radiation therapy can be used pre- or post-surgery to target cancer effectively.
- Common side effects include fatigue, nausea, and skin changes.
- Preparation and knowledge of potential risks can enhance patient engagement.
- Engaging with healthcare providers about side effects is crucial for effective management.
Understanding Radiation Therapy
Understanding radiation therapy is vital for those dealing with lung cancer. It uses high-energy rays to destroy cancer cells. Treatments can be given from outside the body or directly inside it, fitting the cancer’s stage and spot.
The main goals of radiation therapy in treating lung cancer are:
- Shrinking tumors before surgery
- Killing remaining cancer cells post-surgery
- Preventing cancer from spreading
- Relieving symptoms associated with advanced stages of cancer
External beam radiation therapy usually happens five times a week. Each session goes for about 10 to 30 minutes. A machine called the linear accelerator sends beams from different angles, targeting the cancer cells precisely.
Patients might face short-term and long-term side effects. The most common ones are skin issues, nausea, feeling tired, and a sore throat. These usually get better within two months. But, it’s key to watch out for late side effects too.
In cases of small cell lung cancer (SCLC), doctors might suggest prophylactic cranial irradiation. This is to help reduce the risk of the cancer reaching the brain. Getting to know radiation therapy is key for effective lung cancer treatment and outcome management.
How Radiation Therapy Works for Lung Cancer
Radiation therapy is key in lung cancer therapy. It uses high-energy X-rays or particles to target cancer cells. This approach aims to kill tumors while protecting healthy tissues around them.
The process starts with detailed planning and simulation. Doctors use CT scans to find the cancer’s exact location. This ensures the radiation hits its target. Each patient gets a treatment plan that matches their cancer’s specifics.
Radiation therapy has many techniques to make it more effective. Stereotactic body radiation therapy (SBRT) gives concentrated doses quickly, in 5 to 8 days. It’s better at saving healthy tissue than older methods. Intensity-modulated radiation therapy (IMRT) changes the beam’s strength. This allows for higher doses but shorter treatment times. The Fox Chase Cancer Center is known for its skill in IMRT and volumetric modulated arc therapy (VMAT).
Three-dimensional conformal radiotherapy (3D-CRT) sends radiation from many angles, targeting tumors precisely. High dose rate (HDR) brachytherapy puts radiation right into the lung’s airways, making treatment more effective. Image-guided radiation therapy (IGRT) uses images to locate cancer cells during therapy, ensuring high accuracy.
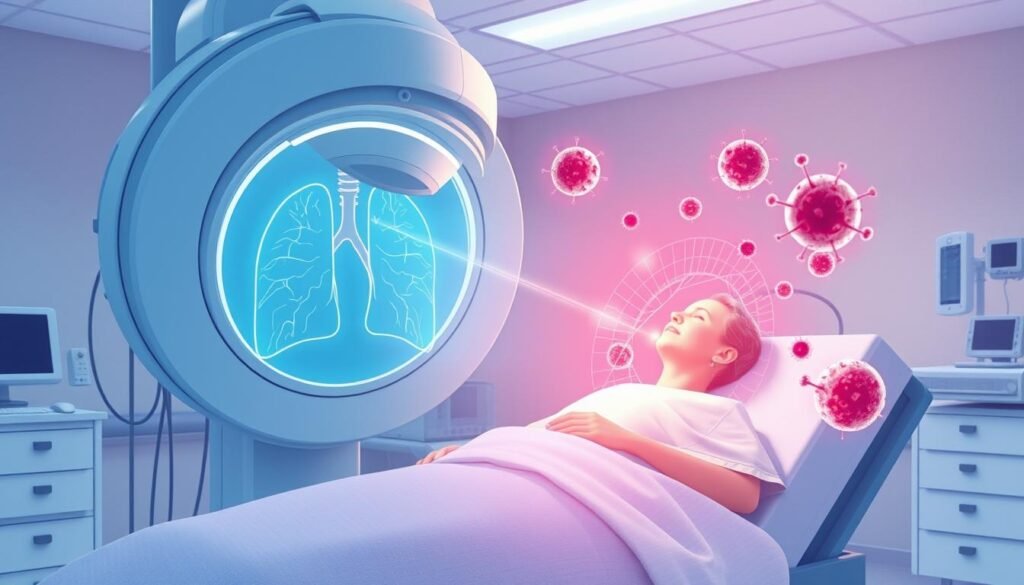
Radiation therapy has several goals. It can try to cure cancer, keep it from coming back, or slow it down. It may also ease lung cancer symptoms, helping improve patients’ lives. Possible side effects include fatigue, and skin irritation. Knowing these helps patients handle their treatment better.
| Radiation Therapy Type | Key Features | Treatment Duration | Benefits |
|---|---|---|---|
| Stereotactic Body Radiation Therapy (SBRT) | High doses over a short period | 5 to 8 days | Preserves healthy tissue |
| Intensity-Modulated Radiation Therapy (IMRT) | Varied intensity beams | Depends on the plan | Higher doses, reduced treatment time |
| Three-Dimensional Conformal Radiotherapy (3D-CRT) | Multiple angle radiation delivery | Varies by case | Precise tumor targeting |
| High Dose Rate (HDR) Brachytherapy | Direct radiation into airways | Immediate | Focused treatment |
| Image-Guided Radiation Therapy (IGRT) | Uses imaging for localization | Daily session variations | Improved treatment effectiveness |
Common Types of Radiation Therapy
Radiation therapy is key in treating lung cancer. It uses methods to best help patients. The common types of radiation therapy include external beam radiation and brachytherapy. Both aim to target tumors effectively while sparing healthy tissue.
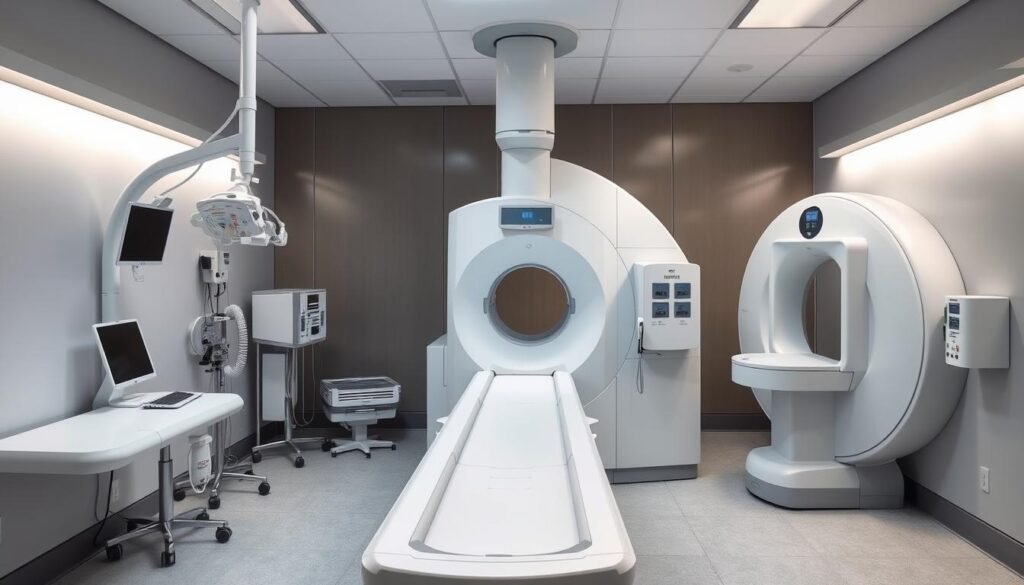
External beam radiation therapy (EBRT) is often used. It targets the tumor with high-energy beams, like X-rays, from outside the body. This method is precise and works for many lung cancer types and stages. EBRT is sometimes used with other treatments, such as chemotherapy or surgery, to improve results.
Brachytherapy is an inside approach. It places radioactive sources close to or inside the tumor. By doing this, it gives a high dose of radiation right where it’s needed while protecting healthy tissues. Brachytherapy is good for certain cancers like those in the head, neck, cervix, and prostate. It’s also used in some lung cancer cases to increase effectiveness.
| Radiation Therapy Type | Procedure | Typical Use | Benefits |
|---|---|---|---|
| External Beam Radiation | Targeted beams from outside the body | Non-small cell lung cancer, advanced cases | High precision; minimizes healthy tissue exposure |
| Brachytherapy | Radioactive sources implanted near or in the tumor | Specific advanced lung cancers | Localized treatment; reduced radiation to surrounding areas |
Knowing about these methods helps in understanding treatment plans. The choice of method depends on the patient’s situation. Factors like tumor size and overall health matter. For more details on treatment options, check out radiation therapy options.
Risks of Radiation Therapy for Lung Cancer Patients
Radiation therapy is a useful option for treating lung cancer. But, it has its risks. Knowing the short-term side effects and long-term complications helps. It allows patients to talk better with their doctors and handle symptoms well.
Short-term Side Effects
Early in radiation therapy, lung cancer patients often face short-term side effects. These include:
- Fatigue, leading to exhaustion over time.
- Nausea, especially when the chest or upper abdomen is affected.
- A sore throat and swallowing issues from tissue irritation.
- Skin redness and irritation in the treated area.
Usually, these side effects are manageable. They tend to go away a few weeks after treatment ends.
Long-term Complications
Patients should know about the long-term complications too. These might show up months or years later. They can include:
- A lingering cough or changes in how you breathe.
- Lowered lung function, affecting your breathing.
- Low blood counts, harming your immune system and needing more care.
- Hair loss where treated, possibly growing back differently.
Late effects depend on where and how much radiation you get. While many face these issues, some treatments can lower the risks.

| Type of Effect | Description |
|---|---|
| Short-term Side Effects | Fatigue, Nausea, Sore Throat, Skin Changes |
| Long-term Complications | Persistent Cough, Reduced Lung Function, Low Blood Counts |
Radiation Pneumonitis: A Significant Risk
Radiation pneumonitis is a big worry for lung cancer patients getting radiotherapy. It’s an inflammation of lung tissues. It can show up as a major problem after treatment. Knowing the signs and how to manage and prevent pneumonitis improves patient health.
Symptoms and Management
Symptoms often start two to three months after radiation therapy ends. You might notice:
- Cough
- Difficulty breathing
- Chest discomfort
To manage these symptoms, doctors often give corticosteroids. These drugs lessen inflammation and help with breathing issues. Other treatments like oxygen therapy and lung rehab also help recovery.
Prevention Strategies
Preventing radiation pneumonitis requires planning before treatment starts. Important steps to stop pneumonitis are:
- Keeping radiation away from the lungs as much as possible
- Using methods that keep the lung dose below 12 Gy
- Watching patients with subclinical interstitial lung disease (ILD) closely, since they’re more likely to get symptoms
Doctors should always check for any early signs of pneumonitis during check-ups. This way, they can work to lessen the chance of it happening. This care can make a big difference in the lives of lung cancer patients.
Radiation Esophagitis: A Common Complication
Lung cancer patients often face radiation esophagitis during their treatment. This condition causes irritation in the esophagus. Patients might experience swallowing difficulties, sore throat, and chest pain. Studies show that the chance of getting acute dysphagia varies, with rates between 13% and 28%.
Higher doses of radiation therapy might lead to more complications. A study on palliative thoracic radiotherapy found dysphagia increased to 20.5% with higher radiation. About 3% of patients may need procedures to open strictures after radical radiotherapy.
Many factors can increase the risk of severe acute esophagitis. These include race, age, gender, overall health, and conditions like gastroesophageal reflux disease. Patients with N2 disease or tumors causing esophageal erosion are at higher risk.
Different radiation therapy techniques affect the rates of acute esophagitis for non-small cell lung cancer patients. The rates for grade 2 or higher esophagitis range from 21% to 75%. Grade 3 esophagitis rates vary between 0% and 70%.
Managing radiation esophagitis usually involves changing the diet, using pain medications, and getting nutritional counseling. Early recognition of symptoms is key. It helps manage symptoms better, greatly improving the patient’s experience during treatment.
| Study Findings | Details |
|---|---|
| Incidence of Acute Dysphagia | 13% – 28% |
| Higher Radiation Therapy Schedules | 20.5% dysphagia compared to 14.9% for lower schedules |
| Strictures Post-Radiotherapy | 3% requiring dilatation |
| Factors for Severe Acute Esophagitis | Caucasian race, age > 70, female, poor initial performance status |
| Incidence of Esophagitis (Grade 2 or Higher) | 21% – 75% |
Radiation-Induced Lung Injury
Radiation-induced lung injury (RILI) is a major concern for lung cancer patients undergoing radiation therapy. The rates of RILI vary widely, from 5% to a high of 58%. This difference comes from several factors like the radiation dose, how the treatment is given, and the patient’s health before treatment.
New treatments such as intensity-modulated radiotherapy (IMRT), volumetric arc radiotherapy (VMAT), and stereotactic body radiation therapy (SBRT) aim to reduce lung cancer treatment risks. These methods target tumors more accurately, cutting down the chance of severe lung damage. About 20% of patients see major lung issues. Yet, daily treatment patients face more toxicity, with 43% experiencing grade 2 or higher toxicity compared to 7% on alternate day schedules.
Several factors increase RILI risk. Patients getting both chemotherapy and radiation see lung damage rates of 32%, much higher than the 6% with only radiotherapy. Chronic obstructive pulmonary disease (COPD) or interstitial lung disease (ILD) also raises this risk. Plus, smokers have a 20% higher chance of developing pneumonitis.
| Risk Factor | Effect on RILI |
|---|---|
| Radiation Dose > 40 Gy | Higher risk of developing RILI |
| Age > 70 years | Increased likelihood of RILI |
| Concurrent Chemo-Radiotherapy | Higher frequency of lung toxicity |
| Location in Mid-Lower Lung | Stronger association with developing pneumonitis |
| Pre-existing Lung Disease | Significantly increases risk |
Understanding how radiation causes lung injury is vital. Ongoing research focuses on better prevention and treatment. This includes precise techniques and possible drugs. For more details, check out this source on the latest in managing RILI from lung cancer treatments. It’s critical to evaluate each patient’s risk to better outcomes and reduce risks.
Coping with Cancer Therapy Toxicity
Dealing with cancer therapy’s harsh effects is key to keeping a good life quality during treatment. Patients face challenges like tiredness, feeling sick, and thinking problems. Knowing about these side effects lets patients help manage their treatment better.
Talking with healthcare teams about side effects can lead to finding good ways to handle them. Supportive care services provide helpful resources and knowledge. They help patients deal with these tough times. Changes in diet can also help with symptoms, making sure the body gets needed nutrients.
Medicines that manage symptoms can help with the harsh effects of cancer therapy. There are medicines for sickness or pain specific to cancer-related issues. Getting support for mental health is crucial too. Being mentally strong can impact recovery a lot. Methods like relaxation or mindfulness can help with feeling emotionally stable.
Using these methods can make going through cancer therapy better. The journey is hard, but open talks and being active in managing side effects can help a lot. Patients can handle the tough parts of treatment with the right support.
Conclusion
Reflecting on the risks of radiation therapy shows us how important it is to make informed choices. This is mostly for lung cancer patients who are considering or going through radiation. Despite its benefits in treating lung cancer and its use in surgery, there’s a real risk tied to it.
This risk includes a higher chance of developing other types of cancer, like those in the stomach and other organs. A detailed lung cancer treatment overview can help patients and doctors weigh the benefits against these risks.
Studies point out that radiation therapy might decrease the risk for some cancers but increase it for others, such as esophageal cancer. Especially in young women, the chance of getting another cancer grows significantly ten years after diagnosis. This fact highlights the importance of continuous care and monitoring even after treatment ends.
Patient and doctor communication is key to better treatment results. When patients and healthcare providers talk openly about the dangers and side effects of radiation, it leads to smarter health decisions. According to research from the Surveillance, Epidemiology, and End Results (SEER) database, ongoing studies are crucial. They will help improve how safe radiation therapy is for lung cancer patients.