Small cell lung cancer (SCLC) makes up about 13-15% of all lung cancer cases. It’s a big concern for public health. In the past, it was thought to represent 20-25% of lung cancer diagnoses. This shows how fast it grows and spreads. This guide highlights how important chest X-rays are in spotting and diagnosing SCLC. Knowing how imaging in oncology works helps healthcare pros make quick, accurate diagnoses. This leads to better results for patients facing this tough disease.
Key Takeaways
- Small cell lung cancer comprises 13-15% of lung cancer cases.
- Chest X-rays play a crucial role in the initial stages of diagnosis.
- Chest radiography has limitations in detecting early signs of SCLC.
- Imaging tests, including PET/CT, are essential for staging lung cancer.
- Timely diagnosis can significantly impact treatment outcomes.
- Understanding imaging modalities is key for healthcare professionals.
Understanding Small Cell Lung Cancer
Small cell lung cancer (SCLC) is a main type of lung cancer, especially dangerous for smokers. It’s often found late and grows quickly. Detecting it early is key to fighting the disease effectively.
Overview of Small Cell Lung Cancer
About 10% to 15% of lung cancers are SCLC. It’s more common in smokers and in men than women. The cancer grows fast and spreads to places like the brain and liver. This leaves patients with very few cure options.
Spotting it early can be life-saving, thanks to methods like x-rays. Knowing the symptoms and risks helps doctors manage it. Things like constant coughing, pain in the chest, and losing weight without trying should be checked out.
Types and Subtypes of Small Cell Lung Cancer
SCLC has two main stages—limited and extensive. Treatment varies a lot between them. Extensive disease often means chemotherapy, radiation, and maybe immunotherapy. Surgery isn’t usually helpful because the cancer spreads quickly.
Clinical trials are crucial for finding better treatments. They help learn about new methods and their side effects, which can include feeling tired, sick, and skin issues.
| Characteristic | Details |
|---|---|
| Incidence | Accounts for 10% to 15% of lung cancers |
| Commonly Affected | More prevalent in smokers, primarily men |
| Treatment Options | Chemotherapy, radiation, immunotherapy |
| Surgery | Rarely effective due to late-stage diagnosis |
| Survival Rate | Low, with few surviving beyond 5 years |
For more insights on early signs and importance of screenings, visit this resource.
Role of Imaging in Diagnosis
Imaging is crucial for diagnosing lung cancer, particularly small cell lung cancer (SCLC). It lets doctors see masses or nodules that might be cancer. This helps decide what treatment to do next. The improvements in thoracic radiology have changed how we detect and watch cancer.
Importance of Diagnostic Imaging
Diagnostic imaging is vital for spotting lung cancer and figuring out its stage. Chest radiographs are often the first step. They show changes in the lung’s structure. If masses are found, doctors use more detailed imaging to learn more.
Imaging Modalities for Lung Cancer Detection
Several imaging methods are used for finding and staging lung cancer:
- CT scans: They give details on the size, shape, and position of lung tumors and lymph node involvement.
- Low-dose CT scans (LDCT): These use less radiation and are better for regular screenings.
- MRI scans: Used to see if cancer has spread to the brain or spinal cord. They provide detailed images but can take up to 50 minutes.
- PET scans: Great for spotting abnormal areas that may be cancer, especially for checking lymph node spread.
- PET-CT scans: These mix PET and CT scans to link metabolic activity with anatomical details closely.
- Bone scans: They are good for finding cancer in bones, but PET scans are often chosen for lung cancer.
About 85 percent of lung cancer tumors are in current or former smokers. This fact shows why regular screenings are important for those at risk. For the best cancer care, knowing how each imaging method helps is crucial.
For more on early detection’s importance, please visit this resource. Imaging tests greatly affect prognosis and treatment options. This makes them an essential part of managing lung cancer. Choosing the right imaging method depends on personal health and what the doctor finds.
| Imaging Modality | Main Purpose | Radiation Exposure |
|---|---|---|
| Chest X-ray | Initial screening for lung masses | Standard |
| CT Scan | Detailed assessment of lung structures | Higher than X-ray |
| Low-dose CT | Lung cancer screening | Reduced |
| MRI Scan | Check for metastasis to the brain/spinal cord | No radiation |
| PET Scan | Identify cancerous lesions/metastasis | Varies |
Each imaging method gives unique insights into lung cancer. They all play a critical role in caring for patients individually.
Small Cell Lung Cancer Xray and Its Limitations
Chest X-rays are often the first step in looking for lung cancer. They are important but not perfect. They especially fall short in finding early lung cancer. It’s key for both doctors and patients to know these limits.
Chest Radiography Effectiveness
Chest X-rays are critical in lung cancer checks. Tumors usually show up as white-grey areas on the images. But, these X-rays can’t always tell cancer from conditions like lung abscesses. Studies show that chest X-rays might miss about 20% of lung cancers. A 2017 study found even higher miss rates for cancers in the upper lobes, between 45% to 81%.
Comparative Analysis with Other Imaging Techniques
Advanced imaging methods like PET-CT scans give a clearer picture than X-rays. They can see active cancer cells better. Different types of biopsies are crucial too. They confirm the cancer’s presence and type, guiding treatment planning.
About 15% of lung cancers are small cell lung cancer. It shows up in two main stages. Treatment usually involves chemotherapy and radiation. Given X-rays’ limits, doctors should use a mix of tests. This will catch lung cancer earlier and improve patient outcomes.
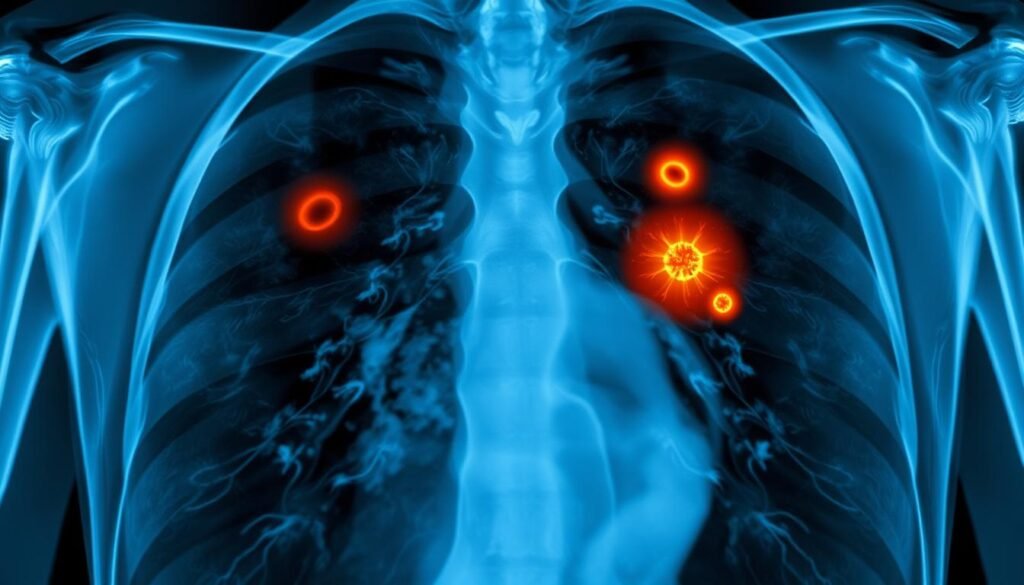
Chest Radiography in Lung Cancer Screening
Chest radiography is key in oncology screening. It’s the first step to check for lung cancer. Though chest X-rays can spot suspicious masses, they can’t confirm cancer. Knowing their strengths and limits is crucial for lung cancer staging and further checks.
The Role of Chest X-ray in Oncology Screening
Chest X-rays are vital in early cancer screening. They help find lung issues. Yet, they often can’t diagnose cancer by themselves. Many studies show that while they hint at further tests, they aren’t great at finding cancer alone.
Limitations of Chest Radiography in Early Detection
Chest radiography has limits in catching lung cancer early. Regular X-rays don’t cut death rates among people. The American Cancer Society prefers low-dose CT scans for those 50 to 80 who smoked a lot. These X-rays use less radiation than CT scans but more than usual X-rays.
The sad fact is, chest radiography can lead to wrong lung cancer calls. About 90% of wrong cancer cases were from X-rays. This shows their limits. Low-dose CT scans are much better, offering clearer views and saving lives by spotting lung cancer better.

| Aspect | Chest X-ray | Low-Dose CT Scan |
|---|---|---|
| Radiation Exposure | Less than standard CT | Small amount, more than chest X-ray |
| Initial Evaluation | Useful, but limited specificity | Highly effective for at-risk individuals |
| Recommended Age | N/A | 50 to 80 with 20 pack-year history |
| Pain Level | Painless | Painless, takes a few minutes |
| Follow-up Requirement | May require additional testing | Detailed images, less follow-up needed |
As we learn more about lung cancer, chest radiography alone isn’t enough. Moving to advanced imaging is in line with current screening advice. It leads to better cancer care strategies.
Lung Tumor Imaging Techniques
Various imaging technologies are key in diagnosing lung cancer today. They have become more accurate, improving our diagnostic tools. This progress helps doctors pick the best treatment plans for patients.
Advances in Imaging Technology
Imaging technology has made big leaps forward in spotting lung tumors. Chest CT scans are especially important. They are very detailed thanks to IV contrast. Further studies show new technologies like 3D reconstructions. These advances make diagnosing even more precise.
Computed Tomography (CT) and MRI in Staging
CT scans are vital in understanding lung cancer better. They tell doctors a lot about the tumor, which helps in planning treatment. MRI is also becoming crucial for this purpose. It’s especially useful for its detailed pictures of thoracic diseases. These tools together give doctors a clear view of cancer and how it grows.
Staging of Small Cell Lung Cancer
Knowing how to stage lung cancer is key for deciding on the right treatment for Small Cell Lung Cancer (SCLC) patients. Staging tells doctors how advanced the cancer is. This decides the treatment plan. The Veterans Administration Lung Study Group (VALSG) and the American Joint Committee on Cancer (AJCC) TNM system are the top staging methods. These methods split cancer into limited and extensive stages.
Overview of Staging Systems
The VALSG system is crucial for planning patient treatment. At diagnosis, one in three people with SCLC have limited-stage cancer. Around two in three have extensive disease. This affects how they are treated. The AJCC TNM system ranks lung cancer from stage 0 to stage IV. It looks at tumor size, node involvement, and if cancer has spread afar.
While TNM is used for SCLC and NSCLC, it’s less vital for SCLC. This complexity means patients should talk to their healthcare providers about their cancer stage and what it means.
Limited vs. Extensive Disease
Differentiating between limited and extensive disease is key in lung cancer staging. Limited-stage SCLC is cancer in one lung and maybe close lymph nodes. Treatment could cure it. Extensive-stage has spread further, affecting other organs. This makes treatment tougher.
Treatment success varies greatly between the two. About 20-25% of limited-stage patients can be cured. Chemotherapy for extensive-stage SCLC can make life better and extend it. But it doesn’t cure. Effective use of staging systems improves treatment results and helps patients through this tough time.
| Staging Category | Description | Prognosis |
|---|---|---|
| Limited Stage | Cancer confined to one lung and nearby lymph nodes. | 20-25% cure rate. |
| Extensive Stage | Cancer that has spread beyond the initial site to other organs. | Improved quality of life and survival, but not curable. |
Diagnosis through Biopsy Techniques
To accurately diagnose small cell lung cancer (SCLC), different biopsy techniques are essential. These techniques help doctors get tissue samples for a clear diagnosis. The method used depends on where the tumor is, how big it is, and how easy it is to reach. This ensures the most accurate diagnosis of lung cancer.
Different Biopsy Methods
Today, we have several biopsy methods for specific cases:
- CT-guided biopsy: Uses imaging to target the tumor precisely.
- Bronchoscopy: Allows doctors to see the airways directly.
- Endobronchial ultrasound (EBUS): Makes bronchoscopy better by showing lymph nodes and tissues around them.
- Navigational bronchoscopy: Improves biopsy accuracy with real-time imaging.
- Surgical biopsy: A surgery to remove lung tissue when other methods can’t.
Importance of Pathological Diagnosis
A thorough pathological diagnosis is crucial in lung cancer cases. It not only confirms cancer but also tells about its type and stage. These details help the medical team make the best treatment plan. Without the right biopsy methods and diagnosis, achieving the best care might be hard.
| Biopsy Technique | Indications | Advantages | Limitations |
|---|---|---|---|
| CT-guided biopsy | Accessible tumors | Minimally invasive | Risk of pneumothorax |
| Bronchoscopy | Central tumors | Direct viewing of airways | Limited to certain lung areas |
| Endobronchial ultrasound | Suspected lymph node involvement | Combines imaging with biopsy | Requires specialized training |
| Navigational bronchoscopy | Peripheral tumors | Enhanced accuracy | Higher cost |
| Surgical biopsy | Indeterminate cases | Comprehensive tissue sample | Invasive with longer recovery |
Monitoring and Follow-Up in SCLC Patients
It’s crucial to monitor patients with Small Cell Lung Cancer (SCLC) closely. Doing so helps catch any signs that the disease is getting worse in time. This allows for better decisions about how to treat the patient.
Having regular scans is key to checking if the cancer might come back. Advanced imaging helps a lot in managing the patient’s care well.
Imaging for Recurrence Detection
Chest CT and PET scans are really important for spotting if SCLC has returned. They can find small changes in the tumor or new spots that show the cancer might be back. This means doctors can change the treatment plan quickly if they need to.
Prognostic Indicators and Treatment Decisions
Some factors are crucial in choosing the right treatment for SCLC patients. This includes how advanced the disease is, whether it has spread, and how well the patient is overall. These factors help doctors predict how well treatments might work and how long the patient might live.
Knowing these indicators helps doctors come up with a care plan. This plan aims to improve the patient’s life and help them live longer.
Conclusion
Chest X-rays are crucial in spotting small cell lung cancer (SCLC). SCLC is amongst the deadliest lung cancers. High-tech scans should supplement X-rays to grasp the full extent of the tumor.
Quick diagnosis plus early treatment greatly help patients. Studies show SCLC often spreads fast. Hence, combining scans with physical exams and biopsies is key. The future looks hopeful for better diagnosis and treatments, thanks to tech improvements. Find out more in this detailed article.
Keeping up with lung cancer’s changing face is critical for doctors. Knowing how to spot and treat SCLC will lead to better care. It is a challenge but also a priority in oncology today.